




Supporting a side sleeping position that keeps the airway open isn’t just about quieting the noise; it’s about promoting healthier,oxygen-rich breathing and improving sleep quality – for both of you!

Gasping for air or the making of choking sounds is the body’s emergency response to not getting enough airflow or oxygen. It’s a reflexive attempt to pull in air when normal breathing has been disrupted enough that the brain has to intervene to restore airflow. This can be a frightening experience for you and your partner. Gasping for air is not a condition itself — it’s a symptom that can signal various underlying issues. One such issue is the narrowing or collapsing of the airway, causing airflow to drop until the brain triggers a fight response and a sudden breath. This is common in snoring and high-risk sleep apnea disorders.
Side sleeping can meaningfully reduce gasping for air when the cause is airway obstruction, as it helps keep the airway open, and reduces the likelihood of breathing interruptions. It’s not a cure for all causes of gasping, but for airway related problems, it’s one of the simplest and most effective changes that can be made.

From your side of the bed, those silent gaps in breathing don’t feel normal — and they’re not. Stopping breathing during sleep is a sleep related breathing
disorder and a key sign of sleep apnea, a condition where the airway repeatedly collapses and airflow repeatedly slows or stops throughout the night. Observing your loved one, you may become aware of several signs, such as long pauses in breathing, snoring followed by silence for a time, gasping or
choking awakenings, and restless sleep. Each pause forces their body to jolt awake just enough to restart airflow, disrupting their sleep and yours. Over time, these interruptions can lower oxygen levels, strain the cardiovascular system, and increase long-term health risks.
Helping them stay in a side-sleeping position that keeps the airway more open isn’t just about reducing the nighttime worry you feel — it’s about supporting steady and rhythmic breathing for them, and healthier sleep for both of you.
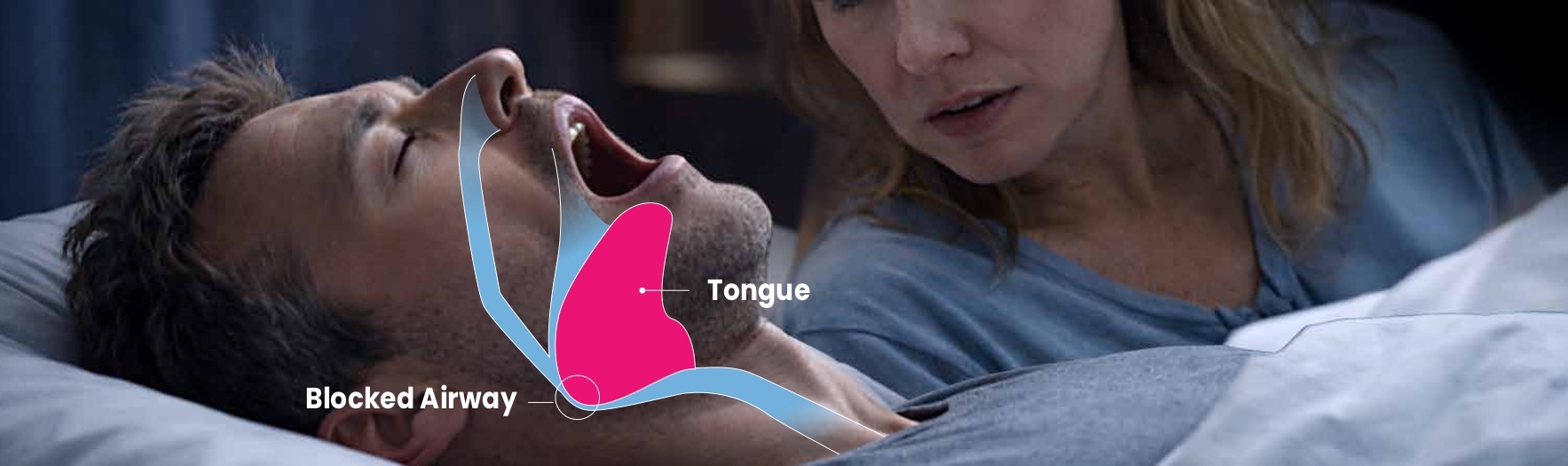
From your side of the bed, those silent gaps in breathing don’t feel normal — and they’re not. Stopping breathing during sleep is a sleep related breathing
disorder and a key sign of sleep apnea, a condition where the airway repeatedly collapses and airflow repeatedly slows or stops throughout the night. Observing your loved one, you may become aware of several signs, such as long pauses in breathing, snoring followed by silence for a time, gasping or
choking awakenings, and restless sleep. Each pause forces their body to jolt awake just enough to restart airflow, disrupting their sleep and yours. Over time, these interruptions can lower oxygen levels, strain the cardiovascular system, and increase long-term health risks.
OSA is a widely undiagnosed sleep disorder in 80 to 90% of the population.
In the U.S., an estimated 30 million adults have clinically significant OSA, yet about 80% – roughly 24 million people – remain unaware of this sleep related threat. Including mild cases, the total may reach 85 million. Globally, 80–90% of people with OSA are undiagnosed. Because untreated OSA carries serious health risks, early screening and effective treatment matter. If you’ve been diagnosed – or suspect you may have sleep apnea—taking action now can protect your long-term health.

You’re not alone in seeing your partner reject CPAP therapy. While CPAP is clinically effective for obstructive sleep apnea, consistant use is a major challenge. Studies show up to 50% of patients never start or stop using CPAP within the first year, often due to discomfort, mask issues, or lifestyle fit. Even among those who begin treatment, 46%–83% are non-compliant, and in mild cases, long-term adherence can drop to about 26% after 12 months. These statistics highlight the limitations of relying solely on CPAP. Research shows that positional therapy can be a viable alternative for CPAP-intolerant patients, particularly those with positional obstructive sleep apnea (POSA).
By keeping patients off their backs and sleeping on their side, positional therapy helps reduce airway collapse and has demonstrated similar reductions in apnea-hypopnea index (AHI) with significantly higher adherence rates. Any decision to discontinue CPAP or transition to positional therapy should be made in consultation with a qualified healthcare professional, as self-directed changes may lead to ineffective treatment and increased health risks.

It’s never too late to take action. Despite clear medical warnings, many people with obstructive sleep apnea (OSA) remain untreated. About 31% of diagnosed patients never begin treatment, and up to 50% of those who start CPAP stop using it within the first year. Overall, roughly one in three people ignore or abandon care, increasing their risk of heart disease, stroke, diabetes, and cognitive decline.
OSA is a widely undiagnosed sleep disorder in 80 to 90% of the population.
In the U.S., an estimated 30 million adults have clinically significant OSA, yet about 80% – roughly 24 million people – remain unaware of this sleep related threat. Including mild cases, the total may reach 85 million. Globally, 80–90% of people with OSA are undiagnosed. Because untreated OSA carries serious health risks, early screening and effective treatment matter. If you’ve been diagnosed – or suspect you may have sleep apnea—taking action now can protect your long-term health.

If you’ve been told that thunderstorms are more peaceful than your snoring, this might get a laugh – but chronic snoring is no joke, as it can signal serious health issues. Chronic snoring refers to frequent or persistent snoring that occurs most nights and can disrupt sleep quality for both you and your loved one. Unlike occasional snoring, chronic snoring may indicate an underlying health issue such as obstructive sleep apnea (OSA) or other airway problems. It happens when airflow through the nose and throat is partially blocked during sleep, causing tissues in the airway to vibrate and produce sound. Sleeping on your side can help reduce chronic snoring and symptoms of obstructive sleep apnea because it keeps the airway more open. When lying on your back, gravity causes the tongue and soft tissues to fall backward, narrowing the airway and increasing obstruction.
In many cases, side-sleeping can prevent this collapse, improving airflow and reducing snoring and apnea episodes – turning that thunderstorm into a quiet whisper, and helping you and your loved one rest easier.
Obstructive sleep apnea (OSA) disrupts the glymphatic system, the brain’s primary mechanism for clearing metabolic waste during sleep. This system is most active during deep sleep, when cerebrospinal fluid removes neurotoxic proteins such as β-amyloid and tau. In OSA, repeated airway collapse
fragments sleep and lowers oxygen levels, impairing glymphatic flow. Imaging studies show reduced glymphatic function in people with OSA, with greater impairment as severity increases. Over time, diminished waste clearance may contribute to Alzheimer’s, dementia, and other neurodegenerative risks, while improvement in OSA has been associated with partial recovery of glymphatic function.
Sleeping on your side has been shown to lower the risk of neurological diseases by enhancing the brain’s waste clearance system.
Nothing says “sweet dreams” like sleeping with a leaf blower strapped to your face. You’re not alone in struggling with CPAP. Masks can feel intrusive,
airflow can cause dryness or bloating, the equipment disrupts natural sleep, and upkeep is a hassle—leading many people to abandon therapy, even though CPAP is effective for OSA.
For some, positional therapy helps. Side-sleeping can keep the airway open, reduce breathing interruptions, and improve sleep quality—especially for positional OSA. In certain cases, combining positional therapy with CPAP allows for lower, more comfortable pressure settings. Any treatment changes should always be made with a qualified healthcare professional.